The immune system is a complex series of barriers, mechanisms and coordinated responses that help the body maintain its natural balance when facing external challenges. It involves a wide range of cells distributed throughout the body, interacting continuously to support appropriate defensive reactions both systemically and locally. Innate immunity provides the body’s first line of support. It includes physical barriers, rapid-response mechanisms capable of recognizing common biochemical patterns, and cellular processes such as inflammation or phagocytosis, which act quickly and broadly to maintain health and balance.
Adaptive immunity is highly specialized, relying on B cells and T cells that recognize specific antigens and enable tailored responses. Although slower than innate immunity, this system is crucial for immune memory and efficient recognition of previously encountered agents.
A well-functioning immune system not only reacts to challenges but also avoids overreaction to non-harmful stimuli and resolves responses when they are no longer required. Supporting this balance contributes to overall immune resilience.
Consuming nutrients such as omega-3 from plant-based, sustainable sources may help support the natural functioning of the immune system while aligning with environmental responsibility.
Given the complexity of the immune system, proper nutrition plays a key role in supporting its proper functioning. Micronutrients such as vitamins and minerals, together with plant-based long chain omega-3 fatty acids (DHA and EPA), are recognized as important contributors to an immune response that remains balanced and well regulated [1, 2]. The importance of nutrition has been recognized since the days of scurvy, although the mechanisms (vitamin C deficiency) took a little longer to work out.
Scientific knowledge of immune function continues to evolve, and the recent focus on viral infections, including SARS-CoV-2, has highlighted the value of supporting the immune system through diet.
Prevention remains central: hygiene practices and vaccination are essential measures to support population health. At the same time, maintaining an adequate intake of key nutrients, including vitamins, minerals, and plant-based omega-3 fatty acids, is recognized as supporting balanced immune function and overall wellbeing [3]. Consuming sustainable, plant-based omega-3 aligns with both individual wellbeing and environmental responsibility, contributing to long-term health outcomes.
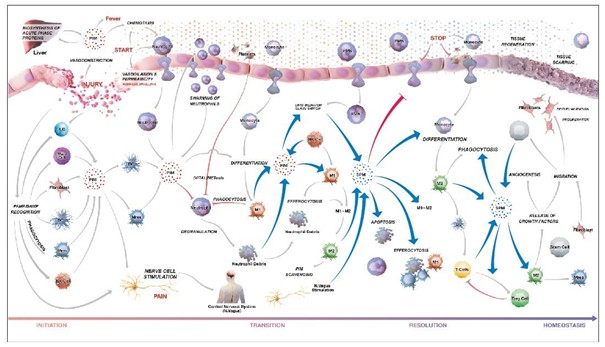
The role of Omega-3s in the immune system
DHA and EPA appear to have at least three major roles in the immune system. Experimental studies on human primary monocytes and T-helper cells show that these fatty acids help the immune system respond appropriately to triggers and return to a resting state after challenges without suppressing its essential activity [5].
While attention is often focused on responding to infections, regulating the immune response after the threat has passed is crucial for long-term health. Chronic unresolved inflammation can have a negative impact on overall wellbeing and quality of life. Studies suggest that plant-based omega-3s from sustainable sources, such as DHA and EPA, support controlled immune responses, helping the system return to balance after challenges [6]. By contributing to the regulation of immune activity, omega-3s clearly have an important role in keeping our well-functioning immune system, without implying treatment or prevention of specific diseases.
Incorporation into immune cell membranes
As we saw in an earlier newsletter on brain and eye health, DHA and EPA play a key structural role in cell membranes. These fatty acids are rapidly incorporated into immune cells membranes, within a day and peaking after a few weeks of supplementation. In the study by Kew et al. (2004), healthy adults received 3.4 g/day of EPA and DHA for 6 weeks, confirming that supplementation can modify immune cell membrane composition. Using plant-based, sustainable omega-3s ensures these benefits are compatible with environmentally responsible and vegan-friendly diets [7].
This incorporation into immune cell membranes helps partially replace arachidonic acid (AA), an omega-6 fatty acid involved in the production of certain pro-inflammatory molecules. Adequate intake of plant-based, sustainable omega-3s contributes to maintaining a balanced inflammatory response, supporting well-regulated immune function [8].
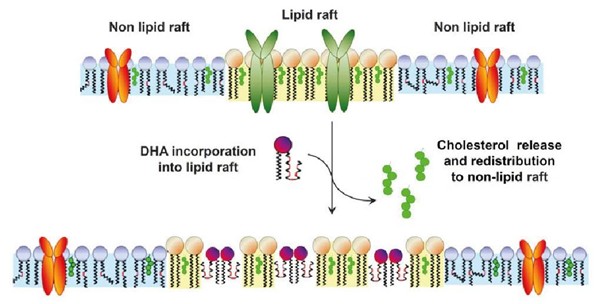
The presence of omega-3 fatty acids, particularly DHA, can influence the organization of immune cells membranes. structure. Specific regions involved in cellular signaling, often structured as protein ‘rafts’ stabilized by cholesterol, can trigger inflammatory signals. DHA has been shown to disrupt these cholesterol-rich rafts, dispersing them and modulating signaling activity [9].
Omega-3 influence on immune gene expression
Beyond their structural role in cells membranes, EPA and DHA influence the expression of genes involved in immune function. In a study of healthy adults aged 65 and older, supplementation with omega-3 providing 1.8 g EPA + 1.0 g DHA per day over 26 weeks altered the expression of more than thousand immune-related genes, with the magnitude of change depending on the dose administered [11]. Roughly half of these genes were downregulated, including those involved in inflammatory pathways and the conversion of arachidonic acid (AA) to pro-inflammatory compounds. This illustrates that EPA and DHA from sustainable, plant-based sources, can have positive effects on immune regulation at the genetic level.
DHA as a precursor for bioactive metabolites
Polyunsaturated fatty acids such as DHA and EPA are not only structural components of cell membranes but also precursors for bioactive molecules, including resolvins, protectins, and maresins that contribute to maintaining balanced and regulated immune responses [12].
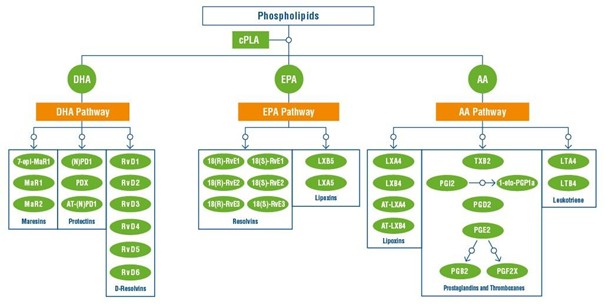
While omega-6 arachidonic acid can generate pro-inflammatory compounds such as prostaglandins, thromboxanes, or leukotrienes, it also gives rise to some inflammation-resolving metabolites like lipoxins. EPA is converted lipoxins and resolvins, that help resolve inflammation, whereas DHA produces three families of bioactives:
- Maresins, supporting the resolution of inflammatory and allergic reactions, aiding tissue repair, and reducing neuropathic pain
- Protectins, with potent anti-apoptotic and anti-inflammatory properties D-Resolvins, which assist in restoring normal cellular function following inflammation.
DHA from sustainable, plant-based microalgae sources provides these metabolites naturally, aligning immune support with environmental responsibility.
Ensuring optimal nutrition for immune health
A growing body of research shows that a well-balanced diet can impact both immediate health and long-term wellbeing, including the immune system. Meeting all nutritional needs while living sustainably and respecting the planet can be challenging, especially for those reducing or avoiding meat and fish. Supplementation with algal DHA offers an effective strategy to ensure adequate intake of these essential fatty acids. In a study on 67 healthy adults, daily supplementation with 450 mg or 900 mg of DHA for 6 weeks significantly increased DHA levels in red blood cells and plasma and also contributed to EPA status [13]. This makes algal DHA a sustainable, vegan-friendly option that supports both nutritional adequacy and environmental responsibility.
Fermentalg’s DHA ΩRIGINS™ range provides highly concentrated algal oils, delivering up to 1g of DHA per day in Europe. This allows formulators and consumers to efficiently enhance DHA intake while supporting plant-based and environmentally responsible choices.
SOURCES

.png)
.jpg)